Weight Loss Drug Battle: Trump Team Blocks Biden's Medicare Coverage Plan
Politics
2025-04-04 23:10:01Content
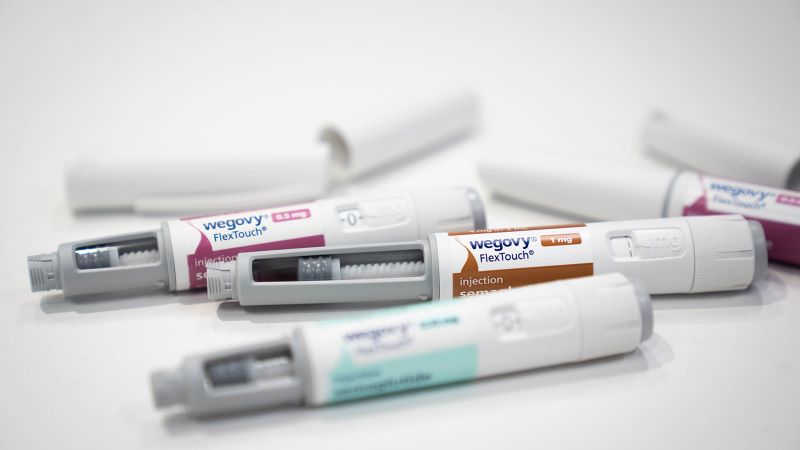
In a significant policy shift, the Trump administration has halted a proposed expansion of Medicare and Medicaid coverage for expensive anti-obesity medications. The decision would have potentially extended access to these costly drugs for over 7 million Americans, but the administration has chosen to block the Biden-era initiative.
This move signals a complex intersection of healthcare policy, pharmaceutical access, and government healthcare spending. By preventing the proposed expansion, the administration has effectively maintained existing restrictions on obesity medication coverage, potentially limiting treatment options for millions of Americans struggling with weight-related health challenges.
The proposal, originally championed during the Biden administration, aimed to broaden the availability of cutting-edge anti-obesity drugs, which can be prohibitively expensive for many patients. By stopping its implementation, the Trump administration has effectively preserved the current, more restrictive approach to obesity treatment coverage under federal healthcare programs.
Medicare's Weight Loss Drug Dilemma: A Policy Shift That Could Impact Millions
In the complex landscape of healthcare policy, the intersection of obesity treatment and government healthcare programs continues to spark intense debate and strategic recalibration. Recent administrative decisions reveal the intricate challenges of balancing healthcare accessibility, cost management, and emerging medical interventions.Transforming Healthcare: When Policy Meets Medical Innovation
The Controversial Landscape of Anti-Obesity Medications
The pharmaceutical realm has witnessed remarkable advancements in weight management medications, with groundbreaking drugs like Ozempic and Wegovy revolutionizing treatment approaches. These medications represent more than mere weight loss solutions; they embody a sophisticated medical intervention targeting metabolic health, insulin resistance, and chronic disease prevention. Researchers have extensively documented their potential to mitigate long-term health complications associated with obesity, including cardiovascular diseases, diabetes, and metabolic syndrome. Healthcare economists and policy analysts have been closely monitoring these developments, recognizing that the integration of such treatments into federal healthcare programs represents a significant financial and strategic decision. The potential expansion of coverage could fundamentally alter healthcare accessibility for millions of Americans struggling with weight-related health challenges.Economic Implications of Drug Coverage Decisions
The decision to halt the proposed expansion carries profound economic ramifications. Anti-obesity medications are notoriously expensive, with monthly treatments potentially costing hundreds or even thousands of dollars. By preventing broader Medicare and Medicaid coverage, the current administration signals a complex calculus of healthcare budgeting and resource allocation. Pharmaceutical companies have invested billions in developing these advanced medications, creating a high-stakes environment where policy decisions directly impact market dynamics. The potential coverage expansion would have represented a transformative moment for manufacturers, potentially opening unprecedented market opportunities for weight management interventions.Patient Perspectives and Healthcare Equity
Beyond financial considerations, the policy shift raises critical questions about healthcare equity and patient access. Millions of Americans, particularly those in lower-income brackets or with complex health histories, could find themselves excluded from potentially life-changing medical treatments. The decision underscores the ongoing challenge of balancing individual health needs with systemic healthcare constraints. Medical professionals have expressed mixed reactions, with some praising fiscal responsibility and others highlighting the potential long-term health consequences of limiting access to advanced metabolic treatments. The debate extends beyond simple cost calculations, touching on fundamental questions of preventative healthcare and systemic wellness strategies.Technological and Medical Innovation Dynamics
The pharmaceutical landscape continues to evolve rapidly, with researchers developing increasingly sophisticated interventions for metabolic health. These medications represent more than weight loss solutions; they are complex biochemical interventions targeting intricate physiological mechanisms. Emerging research suggests that such treatments could potentially reduce long-term healthcare expenditures by preventing chronic disease progression. However, the current policy stance suggests a more conservative approach to integrating these innovative medical technologies into standard healthcare coverage.Future Policy Trajectories
Healthcare policy remains a dynamic, continuously shifting terrain. The current administrative decision does not represent a permanent stance but rather reflects a moment in an ongoing dialogue about medical innovation, healthcare accessibility, and resource allocation. Stakeholders across the healthcare ecosystem—from pharmaceutical researchers to policy makers, medical professionals to patient advocacy groups—will continue to engage in nuanced discussions about the future of metabolic health interventions and their role in comprehensive healthcare strategies.RELATED NEWS
Politics

Graham Warns: Halting Ukraine Aid Could Spark Geopolitical Catastrophe Worse Than Afghanistan Pullout
2025-03-09 17:51:44
Politics

Colorado's Political Landscape Shifts: Bennet's Gubernatorial Ambitions Unveiled
2025-04-10 20:02:11